ABSTRACT
We report a clinical case of adult-onset Still's disease. In addition to the imaging features of the case, the following aspects are also briefly described: clinical presentation (prolonged fever associated with migratory polyarthritis and skin rash), treatment performed (resort to anti-inflammatory and corticoid), and clinical evolution of the patient after having performed the adult-onset.
The treatment was found to be appropriate as the patient presented a favourable clinical evolution.
LEARNING POINTS
- Skin manifestations are associated with systemic diseases.
- Persistent febrile syndromes typically occur in young age.
- Adult-onset Still’s disease is generally considered as a diagnosis of exclusion, as it presents with a combination of non-specific symptoms.
KEYWORDS
Adult-onset Still’s disease, skin rash, fever of unknown origin
INTRODUCTION
First described in 1971, adult-onset Still’s disease (AOSD) is a rare multisystem disorder considered as a complex autoinflammatory syndrome characterised by quotidian fevers, arthritis and an evanescent rash[1,2]. The aetiology of AOSD is unknown. Both genetic factors and a variety of infectious triggers have been suggested as important, but there has been no conclusive evidence to date[1,2].
CASE DESCRIPTION
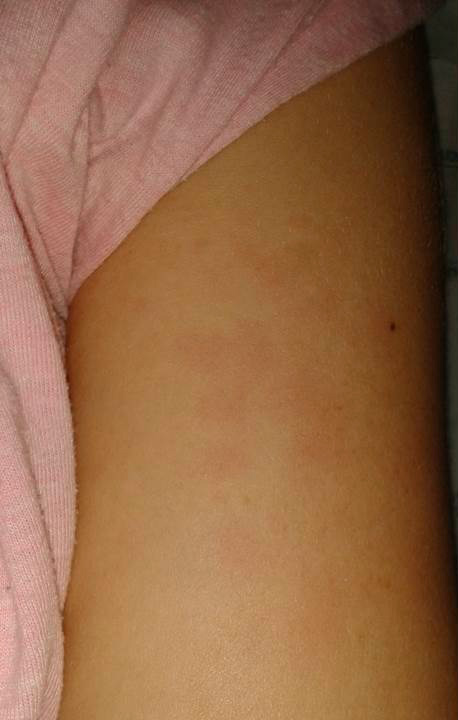
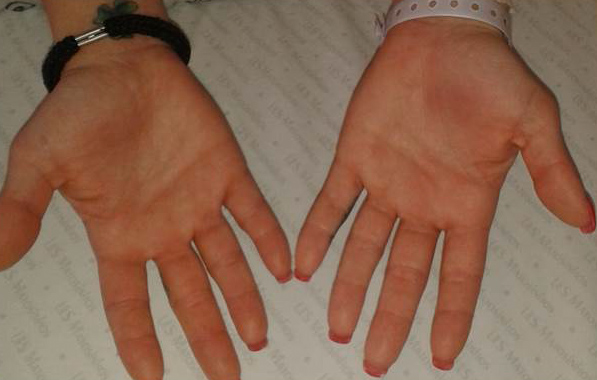
We report an interesting case of a 24-year-old lady who presented with a 10-day history of high spiking fever of unknown origin along with sore throat with cervical lymphadenopathy, evanescent maculopapular salmon-coloured skin rash (over her trunk, abdomen, arms, palms and face – Fig. 1 and Fig. 2), myalgia and migratory polyarthritis. She was found to have neutrophilic leucocytosis (13 500/µL leukocytes and 78% of neutrophils), high serum ferritin levels (20643.45 ng/mL), and elevated erythrocyte sedimentation rate (90 mm/ 1st hour) and C-reactive protein (120 mg/L). She also had abnormal liver function tests hepatosplenomegaly. After extensive workup, potential diagnoses were ruled out and the patient was diagnosed with AOSD based on the Yamaguchi criteria. The potential diagnoses that have been ruled out were neoplastic diseases (eg, lymphoma), insidious infections (eg tuberculosis or zoonosis) or other immune diseases (such as systemic lupus erythematosus). She responded well to indomethacin and was discharged home after 72 hours of apyrexia and symptom improvement. She was readmitted five days following discharge with recrudescence of symptoms.
Subsequently, she was started on high dose prednisolone with clinical improvement and discharged home with outpatient follow-up instructions. At the next clinic visit, all her symptoms had subsided completely and her steroid dosage was tapered appropriately.
Figure 1. Evanescent maculopapular salmon-coloured skin rash on left arm
Figure 2. Evanescent maculopapular salmon-coloured skin rash on palms
DISCUSSION
AOSD still remains a diagnostic dilemma for physicians, as it presents with a combination of non-specific symptoms that can be caused by a wide variety of diseases[1,2].