ABSTRACT
Achenbach’s syndrome, also known as paroxysmal finger haematoma, is a rare condition that results in spontaneous bruising and pain in one or more fingers. Despite its benign and self-limiting course, the remarkable clinical presentation can suggest serious vascular and haematological disease leading to unnecessary referrals and invasive investigations. The authors present the case of a 60-year-old woman with an acute painful and bruised finger. All other physical findings and investigations were normal, except for autoimmune thyroiditis. Based on the clinical presentation and course, the diagnosis of Achenbach’s syndrome was made and the symptoms resolved without treatment.
LEARNING POINTS
- Achenbach’s syndrome is a rare and benign condition characterized by recurrent episodes of sudden pain, bruising and swelling of one or more fingers.
- It is a self-limiting condition and the diagnosis is essentially based on history and clinical examination.
- It is important to recognize this rare syndrome in order to address patient concerns and avoid unnecessary referrals or invasive investigations.
KEYWORDS
Achenbach’s syndrome, paroxysmal finger haematoma
CASE DESCRIPTION
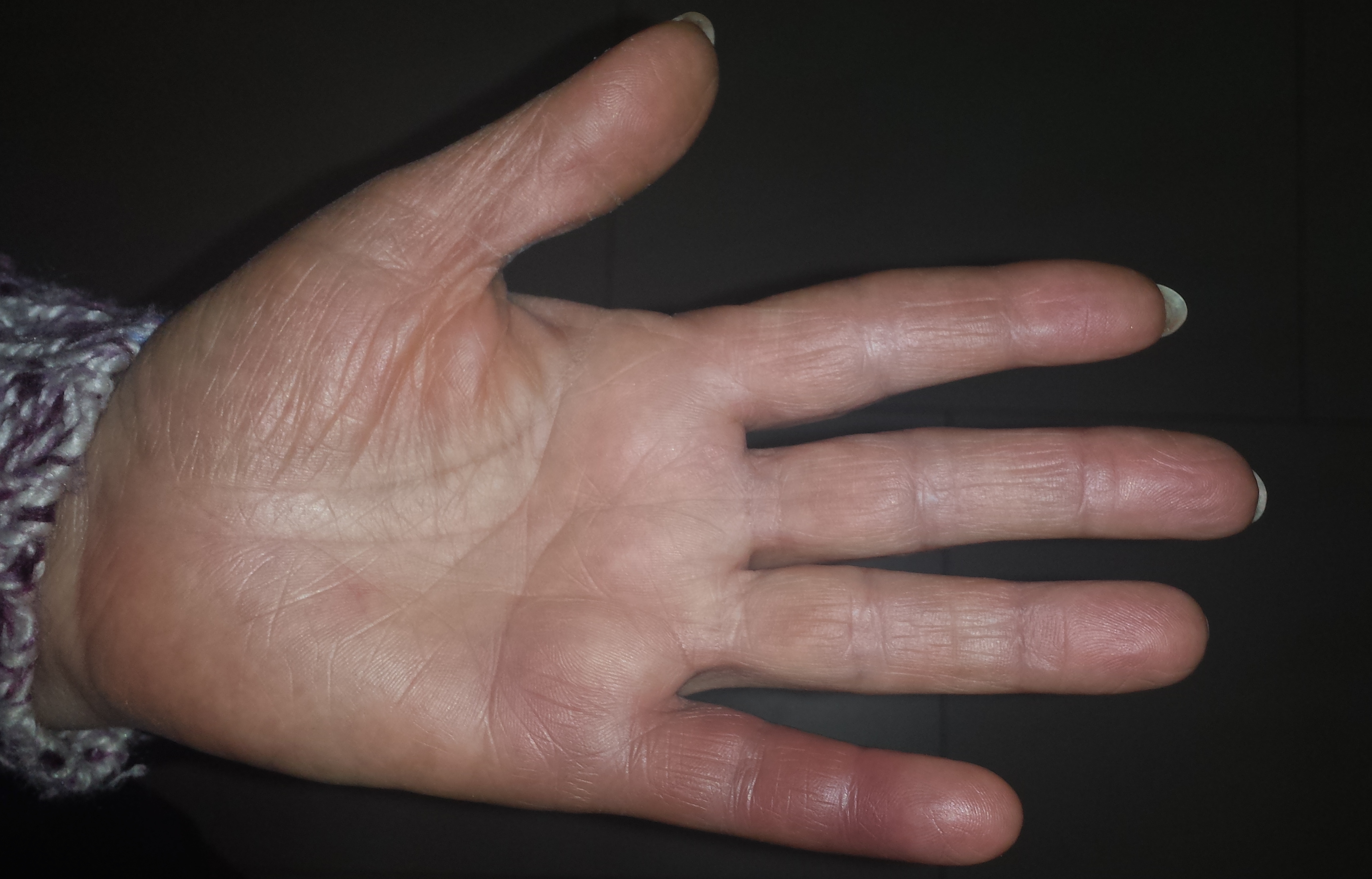
A 60-year-old woman presented to the emergency department with sudden onset of numbness followed by burning pain, swelling and changed colour of the fifth digit of the left hand. No other digits were affected. There was no history of causative triggers such as preceding trauma, cold exposure, stress or medication. Nor were there previous similar episodes or a family history of Raynaud’s phenomenon. The patient was a non-smoker with an unremarkable medical history. On examination the finger was swollen to the level of the metacarpophalangeal joint with bruising over both surfaces of the hand, more intense in the palmar area (Figs. 1 and 2).
The finger was warm and well perfused, without restricted mobility or impaired sensitivity. Allen’s test was normal, brachial, radial and ulnar artery pulses were palpable and symmetric, and there was no difference between blood pressure in the upper limbs. Laboratory tests revealed no platelet deficiency or coagulation disorders, and hand radiography and upper limb Doppler ultrasonography were normal. The patient was discharged without specific treatment and the symptoms resolved within 2 days. Further study with immunological screening revealed autoimmune thyroiditis with subclinical hypothyroidism. The syndrome evolved with recurrent episodes two to three times a year, affecting the same hand region, which resolved completely and spontaneously in a maximum of 3 days.
Figure 1. Palmar view showing the bruised fifth finger
Figure 2. Dorsal view showing the discoloured fifth finger
DISCUSSION
Achenbach’s syndrome, also called paroxysmal finger haematoma or acute idiopathic blue finger, was first described by Walter Achenbach in 1958. It is a rare, benign and self-limiting condition that causes paroxysmal bruising of the fingers. Its prevalence is unknown, although a review published in 2017 by Jiménez et al. mentioned 46 mostly European patients reported since 1973[1], while up to 80 cases might be described in the international literature[2]. Middle-aged women seem to be more commonly affected[1,2].
The pathophysiology of this entity has not yet been established, but as symptoms are typically triggered by everyday activities, increased local vascular fragility, possibly related to age or minor trauma, causing capillary micro-haemorrhages, has been proposed[1–6]. However, many patients develop the disease without an identifiable trigger, as in our patient. Another explanation might be reduced blood flow due to vasospasm or compression by a haematoma. Minor alterations in lower arm arteries have also been reported[2]. Some associations with other diseases such as acrocyanosis, gastrointestinal disorders, gallbladder disease, migraine, goitre and neoplasms have also been noted[1,3,4]. No other reports have associated the condition with autoimmune thyroiditis.
Symptoms are usually described as a burning sensation or pain in one or more fingers followed by purplish or bluish bruising associated with swelling, numbness and sometimes limitation of movement[1–6]. The condition can also be entirely painless[3]. Despite the variable recurrence rate, the disease has a benign course and the bruising disappears spontaneously after a few days, with a mean resolution time of 4 days[1–6]. The most commonly affected region is the palmar surface of the left hand, involving most frequently the index followed by the middle finger, and especially the proximal or medial phalanges. Rare cases may involve the thumb, while there is one report of fifth digit involvement[1].
The diagnosis is essentially based on history and clinical examination, and knowledge of the condition facilitates the diagnosis. Blood counts, conventional radiology and coagulation, autoantibody and vascular flow studies are normal and not useful for the diagnosis, as shown in our case[1–6]. Biopsy specimens may demonstrate non-specific signs such as minor bleeding and inflammation[5]. Minor and non-specific capillaroscopic abnormalities have been reported[4]. However, Achenbach’s syndrome is mainly a diagnosis of exclusion, so diagnostic efforts are aimed at ruling out other conditions. The differential diagnosis includes Raynaud’s phenomenon, acute limb ischaemia, Buerger’s disease, acrocyanosis, vasculitis, Gardner-Diamond’s syndrome and traumatic haematoma.
Kordzadeh et al. proposed a diagnostic algorithm to distinguish between the most common differential diagnoses. The absence of distal pulses suggests acute limb ischaemia. As our patient’s finger had a normal pulse and perfusion, there was no concern about a vascular emergency. If there is a pulse, some other aspects may help the diagnosis: Raynaud’s syndrome is typically associated with the paroxysmal onset of painful, cold and blue-to-white coloured fingers, while patients with acrocyanosis do not report pain and exhibit the iris or Crocq’s sign on examination. In Gardner-Diamond syndrome, changed colouration and pain may affect any part of the body and the condition is associated with personality disorders, nausea, vomiting and bleeding. Lesions that present with pallor, pruritus and ulceration suggest a diagnosis of acrorygosis and chilblains. Finally, the authors propose that Achenbach’s syndrome is indicated by self-limiting episodes of bluish discolouration of the fingers, pain, oedema and paraesthesia in women over 60 years of age with normal limb temperature, no history of trauma and normal Doppler sonography[6].
Due to the benign and self-limiting character of the syndrome, no specific treatment has been proposed. Patients should be counselled about the possibility of symptom recurrence in order to prevent anxiety, as the manifestations of the syndrome may be alarming.