ABSTRACT
Background: Haemangiomas are uncommon chest wall tumours arising outside the rib cage. Their occurrence in intercostal muscle is extremely rare.
Aim: We describe a case of intercostal muscle cavernous haemangioma as a differential diagnosis for chest wall swelling.
Case description: We describe an 18-year-old male patient with an asymptomatic left-sided chest wall swelling. Contrast-enhanced computed tomography revealed a well-defined homogenously non-enhancing mass lesion arising from the seventh intercostal muscle with differential diagnoses of various chest wall tumours. Clinical presentation and imaging findings were inconclusive, but histopathological examination following excision biopsy revealed a cavernous haemangioma. The present case emphasizes the importance of histopathological diagnosis when clinical and radiological examination is inconclusive. Hence, it is necessary to consider intercostal muscle haemangiomas as a differential diagnosis for chest wall tumours in the absence of a feeding vessel.
Conclusion: Despite its rare occurrence, intercostal muscle haemangioma must be considered as a differential diagnosis in chest wall tumours even in the absence of a feeding vessel. We believe that histopathology can provide a definitive diagnosis when most investigative procedures are inconclusive.
LEARNING POINTS
- Haemangiomas are rare chest wall tumours and even rarer when they originate from intercostal muscle.
- Intercostal muscle haemangiomas should be included in the differential diagnosis of chest wall tumours even in the absence of a feeding vessel.
- The present case emphasizes the importance of histopathological diagnosis when clinical and radiological examinations are inconclusive.
KEYWORDS
Cavernous haemangioma, chest wall tumour, histopathology, surgery
INTRODUCTION
Haemangiomas are neoplastic entities arising from blood vessels. They can occur in many parts of the body, with those arising from intercostal muscle being very rare with an incidence of 0.01% of all benign haemangiomas [1]. They usually occur at birth or in the third decade of life, with no sex difference.
CASE DESCRIPTION
An 18-year-old man presented with a 4-month history of an asymptomatic swelling on the left hemithorax. Needle aspiration in the second month was inconclusive but aggravated the size of the swelling and pain developed. Physical examination disclosed a swelling measuring 4×2 cm confined to the left posterolateral aspect of the hemithorax. The plane of the swelling was intramuscular with no obvious thrill palpable or bruit heard on auscultation. A posterior-anterior (PA) chest x-ray showed soft tissue opacity in the left lateral chest wall (Fig. 1). Contrast-enhanced computed tomography (CECT) revealed a well-defined 4.1×1.5×4.2 cm homogeneously non-enhancing lesion in the left lateral chest wall arising from the seventh intercostal space with no feeding vessel, bony erosion or sclerosis (Fig. 2). Thus, the differential diagnoses included glomus tumour, neurofibroma and schwannoma. We did not perform magnetic resonance imaging (MRI) as it was expensive and the lesion was well localized and delineated on CECT.
Figure 1. Chest X Ray
Figure 2. Contrast-enhanced computed tomography of the thorax
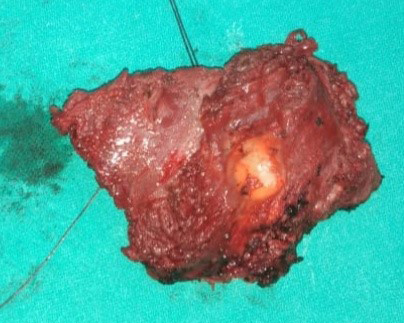
Under general anaesthesia with endotracheal intubation, the patient underwent wide local excision of the swelling with tumour-free margins followed by reconstruction of the resected portion with an overlay of latissimus dorsi muscle. The postoperative course was uneventful. The gross specimen was a grey-brown mass of tissue measuring 6×4.5×4 cm with fatty tissue material with a homogenous yellowish-white appearance on the cut section (Fig. 3). Histopathological examination revealed dilated and congested vascular vessels with fibrous stroma suggesting cavernous haemangioma (Fig. 4). Regular follow-up for a 1 year did not show any recurrence.
Figure 3. Gross specimen
Figure 4. Microscopy demonstrating arteriovenous malformations
DISCUSSION
Chest wall tumours are rare and account for less than 1% of all tumours [2]. Haemangiomas are uncommon and arise outside the rib cage, seldom originating from intercostal muscle. Watson and McCarthy suggested that they are congenital and traumatic in origin [2]. Although chronic liver disease and hormonal imbalance have definite roles in the development of the lesion, a congenital origin is the most common aetiology. Haemangiomas are asymptomatic, but pain occurs as a result of compression of the adjacent intercostal nerve or intervening neurovascular bundle. Histologically, they are categorized into five subtypes: capillary, cavernous, venous, arteriovenous or mixed [3].
Preoperative evaluation with a detailed medical history, clinical examination and radiological investigations is necessary. Imaging, especially CECT and MRI, plays an important role in the diagnosis. CECT for haemangiomas shows a heterogeneous mass with a low level of attenuation due to fatty, fibrous and vascular tissue elements with phleboliths in 30% of cases [4]. The presence of a feeding vessel on CT angiography paves the way for the diagnosis of a vascular lesion. Elbawab et al. [5] in their report demonstrated a vascular mass with a feeding vessel supplied by a branch of the internal mammary artery. Our case presentation was similar to theirs, but the lack of a vascular element in the CT images directed us towards a differential diagnosis of lesions of non-vascular origin. CT of glomus tumours reveals a soft tissue mass with erosion of the adjacent bone. Heterogenous enhancement has been seen with neurofibromas, while with schwannomas, attenuation has been slightly equal to or greater than the muscle [4]. MRI is the preferred modality for the evaluation of chest wall tumours. It can accurately delineate the tumour and enable characterization of tumour tissue. For haemangiomas, MRI demonstrates a homogenous mass with signal intensity similar to that of skeletal muscle on T1-weighted and high signal intensity on T2-weighted images. [2]. For glomus tumours, MRI shows a tumour displacing a major vessel, encircled by tortuous vessels arborizing from a vascular pedicle [4]. The characteristic target sign on T2-weighted images is commonly seen in neurofibromas, and has been reported in up to 50% of schwannomas [4]. Since there is a paradox in the diagnosis of these lesions, histopathological confirmation along with preoperative radiological investigations is of paramount importance. However, when clinical and radiological investigations remain inconclusive, histopathological examination following excision biopsy determines the exact aetiology.
Wide local excision with a tumour-free margin is an accepted treatment of choice [2]. Reconstruction of the chest wall should be considered in lesions involving a major portion of the chest wall (three or more ribs) or an anterolateral defect of more than 5 cm [3]. Various traditional techniques including muscle flap, meshes (biologic/titanium) and methyl methacrylate have been used for chest wall reconstruction, but more recently titanium plates have been used as a prosthetic device as they are biologically inert, less corrosive, resistant to traction and compatible with MRI [6]. Preoperative embolization is palliative and may lead to tumour debulking or reduced bleeding, but surgical excision is mandatory in order to prevent the recruitment of a collateral blood supply [2]. Transformation to malignancy or recurrence is rarely seen.
CONCLUSIONS
Despite their rarity, intercostal muscle haemangiomas must be considered as a differential diagnosis in chest wall tumours even in the absence of a feeding vessel. We believe that histopathology provides a definitive diagnosis when most investigative procedures are inconclusive.