ABSTRACT
Diverticulitis and ulcerative colitis (UC) are two separate colonic pathologies with different underlying mechanisms. Diverticulosis involves herniation of mucosal and submucosal tissue through muscular tissue in response to increased intraluminal pressure. In contrast, it is believed that the muscular tone in patients with UC is reduced due to chronic inflammatory changes. Thus, it has been reported that there may be an inverse relationship between the presence of diverticulosis in patients with UC, in that UC may possibly be protective against developing diverticular disease. Consequently, the co-presence of both pathologies is uncommon. Here we present a case in which a woman with a history of UC and recurrent diverticulitis after elective partial colectomy was admitted for recurrent acute diverticulitis. It is quite challenging to diagnose diverticulitis in ulcerative colitis patients given the usually similar presentation with abdominal pain, diarrhoea and hematochezia. A level of high suspicion is required for diagnosis.
LEARNING POINTS
- Colonic diverticulitis is not commonly associated with ulcerative colitis.
- The diagnosis of colonic diverticulitis in the setting of ulcerative colitis is challenging and requires a high level of suspicion.
KEYWORDS
Colonic diverticulitis, ulcerative colitis
CASE DESCRIPTION
A 47-year-old woman with a medical history of ulcerative colitis (UC), diabetes mellitus and hypertension, and recurrent diverticulitis after partial left-sided hemicolectomy 5 years previously, presented to the emergency department for left lower quadrant abdominal pain associated with bouts of alternating constipation and blood-streaked dark brown diarrhoea. She denied any nausea or vomiting or any other significant symptoms. Her vital signs showed a blood pressure of 115/65 mmHg, heart rate of 96, respiratory rate of 18, temperature of 36.7°C, and oxygen saturation of 96% on room air Physical examination was remarkable for left lower quadrant abdominal tenderness with no rebound tenderness. Initial laboratory work-up was significant for leucocytosis with WBCs 13.9 K/µl. A CT scan of the abdomen and pelvis with contrast showed inflammatory fat stranding and a small amount of fluid in the left lower quadrant between the left aspect of the uterus and the sigmoid colon, in a region with diverticula, findings consistent with acute sigmoid diverticulitis (Fig. 1). Our patient was managed with mesalamine for UC and started on ceftriaxone and metronidazole, bowel rest, intravenous fluids, and analgesia. During hospitalization, inflammatory markers reduced but with initial persistence of symptoms eliciting a repeat CT scan of the abdomen on hospital day 4 which showed sigmoid colon diverticula with improvement of the diverticulitis (Fig. 2). The patient was started on a clear liquid diet and with tolerance transitioned to a consistent carbohydrate diet without any complications. The patient was then discharged on oral antibiotic therapy.
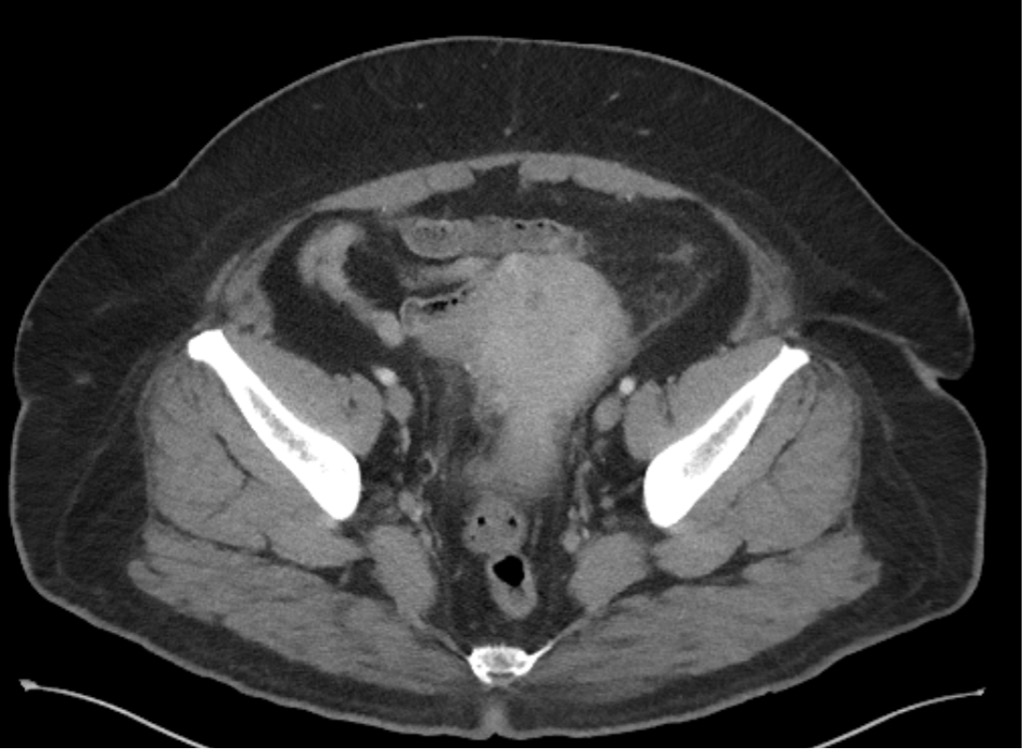
Figure 1. CT scan of the abdomen showed colonic diverticulosis with sigmoid involvement. New inflammatory fat stranding in the left lower quadrant is seen between the left aspect of the uterus and the sigmoid colon
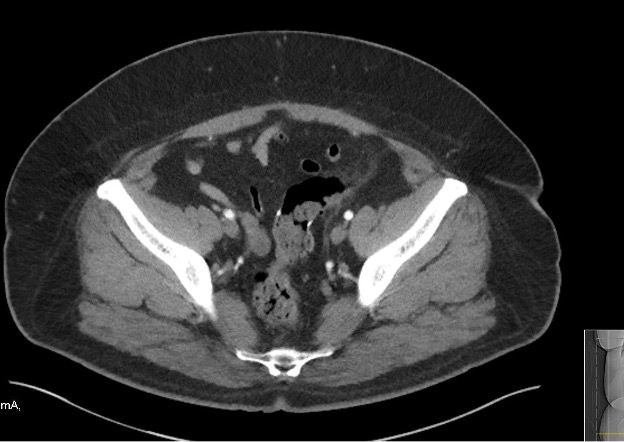
Figure 2. CT scan of the abdomen shows colonic diverticula with no diverticulitis
DISCUSSION
Colonic diverticulosis is an outpouching of the mucosa and submucosa through the circular muscle layer of the colon [1] due to increased intraluminal pressure and sigmoid contractility, causing mucosal herniation at vascular perforation sites [2]. Its prevalence increases with age, reaching up to 70% in adults over 80 years of age. Its presentation is related to risk factors such as obesity and hypertension, and can be prevented or delayed with protective factors like a high fibre diet [3]. When inflammation of diverticula occurs, it is defined as acute diverticulitis, which presents as left hemiabdomen pain, alteration in bowel habits, leucocytosis and fever [1].
Abdominal CT is the test of choice for confirmatory diagnosis of diverticulitis, although not required in uncomplicated patients with mild symptoms.
In contrast, UC is a chronic inflammatory disorder of the colonic mucosa which predisposes to a reduction in both bowel wall muscle tone and contractility. Diarrhoea and blood in the stool are the most common presenting symptoms of UC, which often presents with alternating periods of remission and relapse[4]. Diagnosis is based on clinical symptoms confirmed by objective findings from endoscopic and histological examinations showing continuous colonic inflammation starting in the rectum; rectal sparing is sometimes observed. Histologically, it is usually limited to the mucosal layers with Paneth cell metaplasia, mucin depletion, distortion of crypt architecture, crypt abscesses, and infiltration of the mucosa by lymphocytes, plasma cells and granulocytes [5].
Their pathophysiological mechanisms and effect on bowel pressure and contractility suggest these two entities counter one another, supporting the low frequency of their co-occurrence [6]. One proposed explanation for this decreased frequency is that the presence of chemical mediators, such as interleukin-1b and nitric oxide, cause muscular relaxation in UC, thus decreasing the intraluminal pressures required for diverticula formation [7], and functionally serving as a protective factor with a 3.5-fold decreased risk of diverticula in patients with UC [6].
In our case, we managed a 47-year-old woman with a history of UC, presenting with haemorrhagic diverticulitis which was promptly resolved with supportive therapy. Only 0.3% of patients with either UC or diverticulitis have both conditions simultaneously[8], significantly lower when compared to controls of the same age and gender. Although advancing age is a risk factor for diverticulosis, in UC patients diverticulosis frequently presents late and is associated with a less aggressive UC clinical course. Another possible confounding factor in our patient is the concomitant administration of mesalamine, given that some authors have described a possible inverse correlation between maintenance therapy for UC, for instance with 5-ASA compounds, and diverticula formation [5, 8].