ABSTRACT
We present the case of a 55-year-old man with a self-limiting febrile condition associated with polyserositis with an inconclusive investigation. Bilateral pleural and pericardial effusions resolved. The peritoneal fluid loculated and was compatible with an exudate. The patient remained clinically asymptomatic. However, 2 years later, examination revealed a palpable and painless abdominal mass, which imaging suggested a cystic lesion. Surgical resection was performed and histological examination identified a mesenteric pseudocyst.
Mesenteric pseudocysts are rare intra-abdominal cystic masses which are mostly benign and do not cause specific symptoms. Although imaging tests are useful for their differential diagnosis, histology is mandatory.
LEARNING POINTS
- Mesenteric pseudocysts are rare intra-abdominal cystic masses with a clinical presentation that sometimes is a diagnostic challenge.
- Abdominal imaging used to investigate a concomitant systemic illness may reveal a fluid lesion which may delay the diagnosis.
- Ultrasound, computed tomography and magnetic resonance imaging can be used for pre-operative diagnosis, but exact differentiation is only achieved through histopathological examination.
KEYWORDS
Mesenteric pseudocyst, peritoneal fluid, abdominal cyst.
CASE REPORT
The authors describe the case of a 55-year-old man, a smoker (15 pack-years) with no other previous relevant diseases who presented with a 3-week history of dyspnoea, orthopnoea and dry cough. Examination showed low grade fever (37.8°C) and bilateral decreased breath sounds. Thoracic radiography showed blunting of both costophrenic angles, and a discrete infiltrate in the inferior right pulmonary lobe. Thoracentesis revealed an effusion with exudate characteristics and with 240/mm3 predominantly mononuclear cells. Microbiological cultures and also direct examination and cultures for tuberculosis were negative. The patient was admitted under the diagnostic hypothesis of pneumonia, and amoxicillin/clavulanic acid and azithromycin were initiated.
Further echocardiographic investigation showed a discrete pericardial effusion with no other alterations. Abdominal ultrasound revealed perihepatic and perisplenic fluid. Blood tests revealed high levels of inflammatory markers but no other relevant findings.
The patient was afebrile on the second day of admission and became asymptomatic with full symptomatic recovery.
Further investigation of polyserositis of unknown aetiology was pursued in ambulatory consultation. Neoplastic, infectious and inflammatory causes were ruled out.
Blood tests were normal, there was no urinary proteinuria, and upper gastroesophageal endoscopy and colonoscopy were unremarkable. Antinuclear antibodies were negative. Viral serologies and tuberculous screening were negative. Thoracic tomography revealed scarce pericardial fluid and scant bilateral pleural fluid. Abdominal tomography revealed peritoneal free liquid, with no apparent collections.
Pleural and pericardial effusions resolved and follow-up thoracic radiography and echocardiography showed no signs of either. Repeated abdominal ultrasounds continued to indicate abundant peritoneal fluid, mainly in the right quadrants, with the appearance of loculation and formation of pouches. Guided paracentesis revealed an exudate, with 870/mm3 cells (55% polymorphonuclear cells), negative microbiological cultures, and no other relevant analytical characteristics.
The patient remained asymptomatic, with occasional complaints of discomfort in the right abdominal quadrants when sitting, and under ambulatory surveillance.
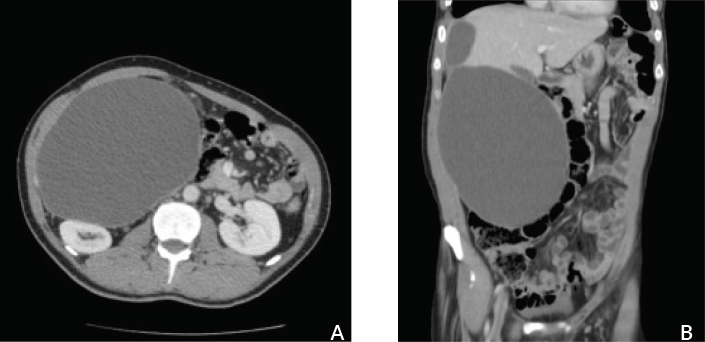
Two years later, at ambulatory consultation, a hemiabdominal swelling was observed at physical examination in dorsal decubitus, which had not been noticed by the patient. A painless right abdominal mass was observed at abdominal palpation, with very little mobility. Analytical studies were normal. Abdominal ultrasound revealed a fluid collection from the inferior low hepatic border to the right iliac fossa (24×17 cm). Abdominal tomography showed a liquid formation with a thin wall, in the right abdominal quadrants, from the right low diaphragmatic level to the umbilical level, with an upper component with a 9 cm axis and an inferior component measuring 21×15 cm (Fig. 1). Several other differential diagnoses emerged. Eccinococcus and Entamoeba histolytica serologies were negative. Abdominal magnetic resonance revealed a cystic lesion in the right abdominal quadrants (30×17×12.5 cm), independent of the liver, and compressing the inferior vena cava and causing leftward deviation of the abdominal aorta (Fig. 2).
Figure 1 (A,B): Abdominal CT scan showing a thinwalled lesion containing liquid and extending from the right infradiaphragmatic level, over the right edge of the liver, to the umbilical level.
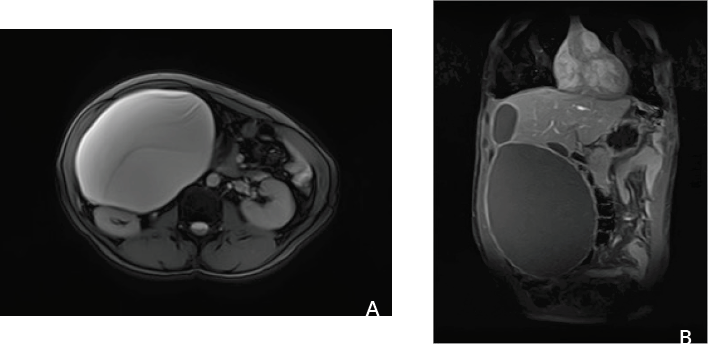
Figure 2 (A,B): Abdominal MRI showing a large cystic lesion measuring 30×17×12.5 cm, independent of the liver, compressing the inferior vena cava and pushing the abdominal aorta to the left.
The patient underwent surgical excision of the lesion: laparoscopy turned into laparotomy due to the size of the lesion and the multiple and tight adhesions which hindered the procedure. No signs of pancreatic, gallbladder or appendix pathology were noted. The patient had an uneventful postoperative course and remained asymptomatic for the following 7 months of follow-up.
Histological examination revealed a mesenteric pseudocyst, with inflammatory infiltrate with a predominance of mononuclear cells.
DISCUSSION
Mesenteric cysts are rare intra-abdominal masses[1] of unknown origin[2]. In adults, they occur primarily in the fourth decade of life[3], with an incidence of approximately 1 in 100,000–250,000 hospital admissions[2], and with almost equal incidence in both genders[1]. They are histopathologically classified as cysts of lymphatic origin, cysts of mesothelial origin, enteric cysts or enteric duplication cysts, cysts of urogenital origin, dermoid cysts and pseudocysts (infectious, traumatic or degenerative)[4].
Mesenteric pseudocysts are challenging to diagnose, since they often present as a disappearing mass or with a changing location[2]. Usually the patient has no symptoms, and the cyst is discovered incidentally on abdominal imaging for other causes. The larger lesions may cause abdominal pain, discomfort, distension or other non-specific symptoms[2].
In our case, the initial presentation together with a febrile illness that caused pleural and pericardial effusions confounded and delayed the diagnosis until the clinical presentation and imaging revealed a defined collection.
Mesenteric pseudocysts may be secondary to trauma or infection[5], and the internal appearance is important in identifying cyst aetiology. In our case, there was an inflammatory infiltrate, and as the patient had no history of trauma, an infectious cause was possible. If the responsible infectious stimulus was the initial described event or another previous, unnoticed one, is unclear.
The treatment is surgical resection, which is also the only way to ensure that the lesion does not develop into a malignant mesenteric cyst as found in 3% of cases[5].