ABSTRACT
A 45-year-old Japanese woman presented with difficulty moving her left shoulder. Ten months previously, the day after she had received her second dose of the BNT162b2 mRNA COVID-19 vaccine, a severe stabbing pain occurred in her entire left upper extremity. The pain resolved within 2 weeks, although she developed difficulty moving her left shoulder. A left winged scapula was observed. Electromyography showed left upper brachial plexopathy with acute axonal involvement and abundant acute denervation potentials, consistent with Parsonage-Turner syndrome (PTS). PTS should be considered in patients with post-neuralgic motor paralysis of the unilateral upper extremity, which can occur after COVID-19 vaccination.
LEARNING POINTS
- Parsonage-Turner syndrome (PTS), also referred to as idiopathic brachial plexopathy or neuralgic amyotrophy, is characterized by acute onset of unilateral upper extremity pain.
- PTS often results in a winged scapula due to paralysis of the long thoracic nerve.
- PTS should be considered in patients with post-neuralgic motor paralysis of the unilateral upper extremity, which can occur after COVID-19 vaccination.
KEYWORDS
COVID-19 vaccination, Parsonage-Turner syndrome, winged scapula
INTRODUCTION
Parsonage-Turner syndrome (PTS), also referred to as idiopathic brachial plexopathy or neuralgic amyotrophy, is characterized by acute onset of unilateral upper extremity pain[1]. The pain resolves within several days to 2 weeks[1]. Thereafter, muscle atrophy and motor paralysis develop in the ipsilateral side[1]. The exact pathophysiology of PTS is hypothesized to include immunological, biomechanical and genetic factors[2]. It is a rare sequela of viral infection, surgery and vaccination[2]. We describe the clinical course of a case of PTS in order to contribute to knowledge of this syndrome occurring after COVID-19 vaccination, and present a review of the literature.
CASE DESCRIPTION
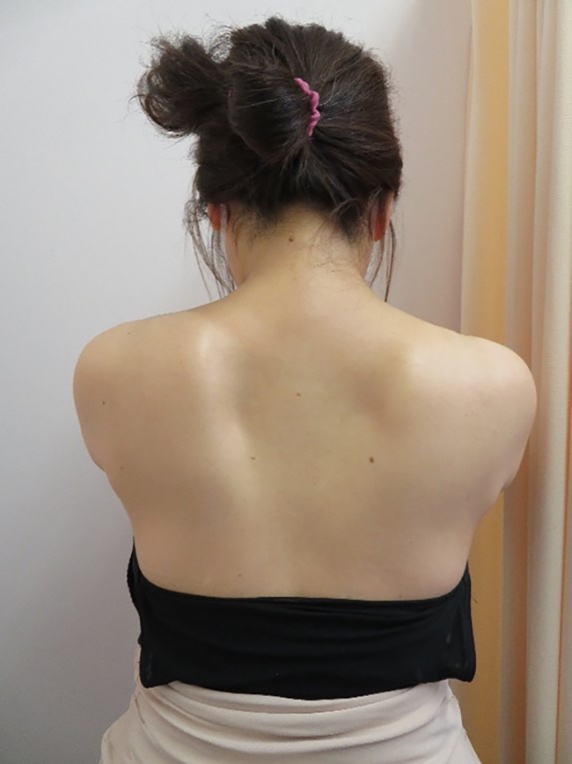
A 45-year-old Japanese woman presented with difficulty moving her left shoulder. Ten months before, the day after she had received her second dose of the BNT162b2 mRNA COVID-19 vaccine, a severe stabbing pain occurred in her entire left upper extremity. The pain resolved within 2 weeks, although she developed difficulty moving her left shoulder. Her past history was unremarkable. She denied antecedent trauma. Manual muscle testing showed weakness in the left deltoid muscle and supraspinatus muscle. A left winged scapula was observed (Fig. 1). There was no evidence of sensory disturbance. Tendon reflexes were normal in the extremities, and pathological reflexes were negative. Electromyography (EMG) showed left upper brachial plexopathy with acute axonal involvement and abundant acute denervation potentials, consistent with PTS. Her symptoms resolved in 2 months after rehabilitation.
DISCUSSION
PTS, also referred to as idiopathic brachial plexopathy or neuralgic amyotrophy, is characterized by the acute onset of unilateral upper extremity pain[1]. The pain resolves within several days to 2 weeks followed by muscle atrophy and motor paralysis ipsilaterally[1]. The most commonly affected muscles are proximal muscles including the supraspinatus, infraspinatus, anterior serratus, deltoid and biceps brachii[2]. The affected nerves are often branches of the brachial plexus such as the suprascapular nerve, dorsal scapular nerve, long thoracic nerve, axillary nerve, musculocutaneous nerve, and anterior/posterior interosseous nerve[2]. In addition, PTS often results in a winged scapula due to paralysis of the long thoracic nerve[2].
Winged scapula is divided into two categories, medial and lateral, according to the direction of winging. Medial winging is more common, being caused by serratus anterior paralysis[3]. This is typically due to damage of the long thoracic nerve[3]. This nerve supplies the serratus anterior, which is located on the side of the thorax and acts to pull the scapula forward. Serratus anterior palsy is a dysfunction that is characteristic of traumatic, non-traumatic and idiopathic injury to the long thoracic nerve[3]. The second category is lateral winging, which is caused by injury of the spinal accessory nerve. Severe atrophy of the trapezius is seen with accidental damage to the spinal accessory nerve during lymph node biopsy of the neck. There are numerous ways in which the long thoracic nerve can sustain trauma-induced injury. These include blunt trauma (e.g., blow to the neck or shoulder, sudden depression of the shoulder girdle, unusual twisting of the neck and shoulder), repetitive movements (as observed in athletic activities such as weight lifting or sports that involve throwing), excessive compression of the shoulder area by straps (backpack palsy), and various household activities (e.g., gardening, digging, car washing, prolonged abduction of the arms when sleeping, propping up the head to read, etc.). Clinical treatments may also cause injury to the long thoracic nerve (iatrogenesis from forceful manipulation, mastectomy with axillary node dissection, surgical treatment of spontaneous pneumothorax, post-general anaesthesia for various clinical reasons, and electrical shock, amongst others)[3]. Non-traumatic induced injury to the long thoracic nerve includes causes such as viral illness, vaccination, allergic drug reactions, drug overdose, toxic exposure, C7 radiculopathy, and coarctation of the aorta[3].
The exact pathophysiology of PTS is hypothesized to include immunological, biomechanical and genetic factors[2]. It is a rare sequela of viral infection, surgery and vaccination[2]. As such, PTS can occur after COVID-19 infection or vaccination[2,4,5]. A postulated mechanism for the development of PTS after COVID-19 vaccination could be related to a reactive inflammatory response[6]. In PTS, EMG typically demonstrates multi-focal acute axonal lesions[2]. Our case is similar in that we found EMG changes in the affected extremity[6]. A limited number of previous case reports linking PTS to COVID-19 vaccination have reported similar physical exam findings of atrophy of the shoulder girdle muscles, decreased force in anterior elevation, abduction, external rotation and internal rotation, as well as denervation and fibrillation potentials findings in EMG studies of the shoulder muscles[5–8]. In addition, it is important to keep in mind that this presentation has been reported to occur within days of vaccination rather than weeks as seen in association with COVID-19 infection[5,7,8].
In conclusion, PTS should be considered in patients with post-neuralgic motor paralysis of the unilateral upper extremity, which can occur after COVID-19 vaccination.