ABSTRACT
There has been a recent outbreak of monkeypox in the United States, mostly among men who have sex with men (MSM). It seems to be a self-limiting disease but can be potentially serious in immunocompromised patients. Monkeypox infection is transmitted mainly through skin-to-skin contact and possibly seminal and vaginal fluids. Very few cases of monkeypox infection in immunocompromised patients have been published in the literature. We report a case of infection in a renal transplant recipient, and describe the clinical course and outcome.
LEARNING POINTS
- There has been a recent outbreak of monkeypox infection in the United States and more studies are needed to assess the disease course in different patient populations.
- Monkeypox infection seems to have a similar clinical course in renal transplant recipients as in the general population.
- There is a higher risk of transmission among renal transplant recipients in men who have sex with men.
KEYWORDS
Monkeypox, renal transplant recipient, sexually transmitted disease
INTRODUCTION
An outbreak of the rare viral disease monkeypox began in May 2022[1]. Monkeypox is a close relative of the human smallpox virus, and both viruses belong to the Orthopoxvirus genus. Although monkeypox is primarily a disease of animals, including monkeys, rats and squirrels, humans can contract the virus through direct contact with infected animals or through consumption of contaminated meat[2]. Young men were the initial victims of the monkeypox outbreak[3]. However, there are public health concerns regarding spread of the infection into the general population, including immunosuppressed transplant patients. Very few cases of monkeypox infection have been reported in transplant recipients in the literature, so the clinical course of the infection in such patients is rarely discussed[4]. Here, we describe the case of a 30-year-old man with end-stage renal disease (ESRD) after renal transplantation, who was infected with the monkeypox virus.
CASE DESCRIPTION
The patient was a 30-year-old man with a medical history of primary syphilis and ESRD due to focal segmental glomerulosclerosis after cadaveric renal transplantation. He was on immunosuppressant medication and had previously been on haemodialysis for 7 years. The patient was admitted to hospital for diffuse vesicular lesions which had been present for over 2 weeks. He stated that he had unprotected anal intercourse with a male partner a couple of days prior to the appearance of the lesions. Of note, the patient is sexually active with men with a history of multiple sexual partners. The patient works in an airport as a customer service agent and did not recall any of his co-workers having such lesions.
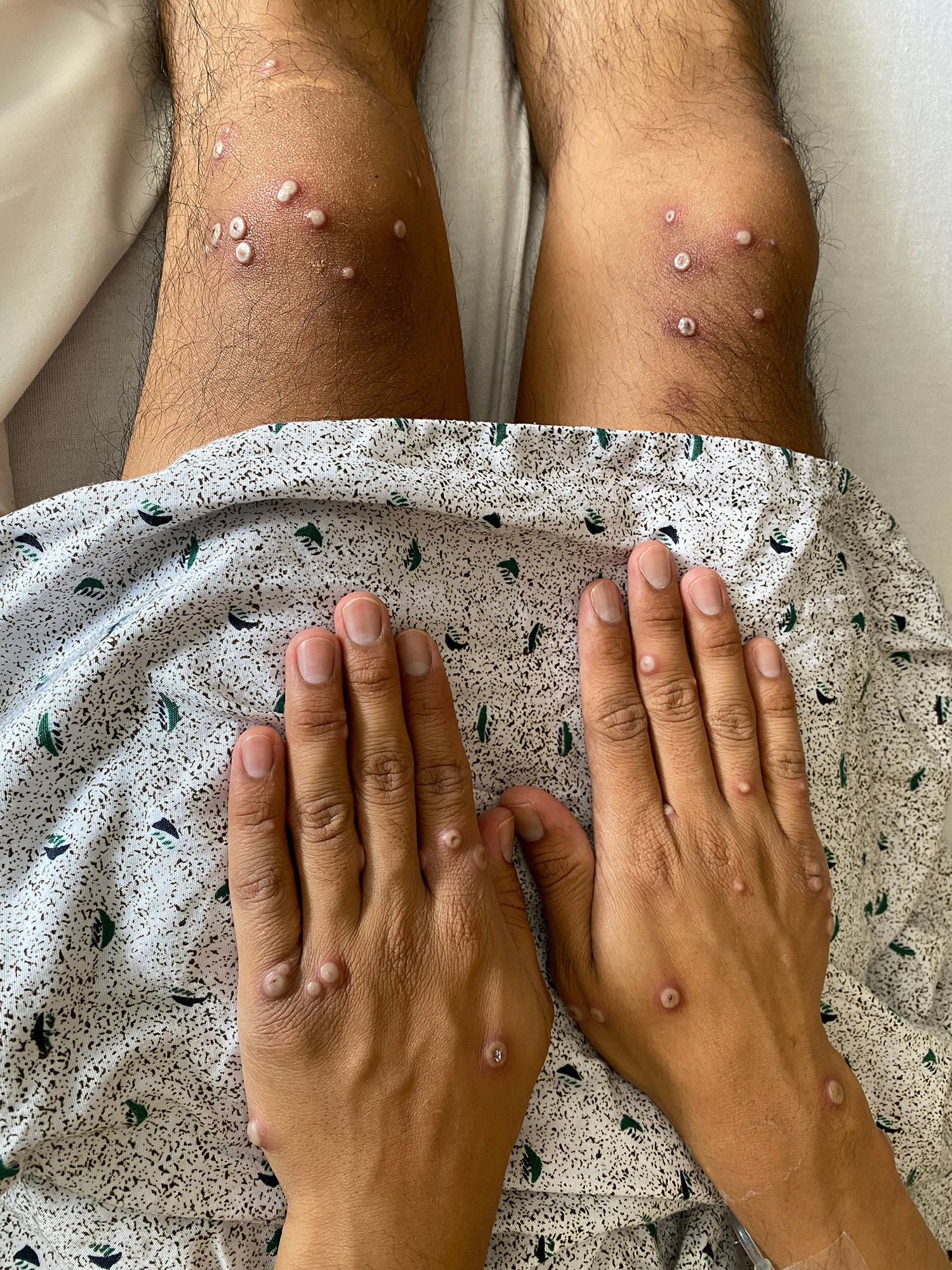
The lesions started on his hand and then spread all over his body including his rectum, genitalia and back, with mucosal involvement including large lesions on his tongue. The lesions were large, firm, raised and umbilicated, indurated and had well-circumscribed borders (Fig. 1). The lesions were scraped for testing and the patient was sent home and told to quarantine pending the results. However, as he was having difficulty swallowing due to pain, fever and worsening lesions, he decided to return to the Emergency Department after which he was admitted to hospital.
He was afebrile, on room air, and his white cell count was 14,400/µl. Blood and urine cultures were negative. A chest x-ray showed no evidence of acute cardiopulmonary disease. Infectious disease work-up was negative for HIV, chlamydia, gonorrhoea, hepatitis and BK virus. However, the PCR test for monkeypox virus was positive. The patient was then started on tecovirimat. He was discharged home, quarantined and completed a 14-day course of tecovirimat. He gradually improved with full resolution of the lesions after about 4 weeks.
DISCUSSION
There has been a recent monkeypox outbreak in the United States with the very few reported cases in the literature mostly in immunocompetent patients. However, some rare cases have been reported in the immunosuppressed population[5]. Renal transplant recipients are immunocompromised due to the use of immunosuppressive medications to prevent organ rejection. As a result, they are more susceptible to infection and have a higher risk of developing subsequent complications. One of the modes of transmission of monkeypox in renal transplant recipients is through sexual contact with an infected partner. Therefore, it is important for renal transplant recipients to practice safe sex and inform their sexual partners of their immunocompromised status to reduce the risk of transmission. Treatment of monkeypox in renal transplant patients is mainly supportive, but antiviral medications can also be used to shorten illness duration and reduce symptom severity. However, the efficacy of these medications in renal transplant patients is not well established, and further research is needed to determine their effectiveness in this population. There was no evidence of increased severity of monkeypox infection in our renal transplant recipient. However, further studies are needed establish the course of the disease in immunocompromised patients.