ABSTRACT
Immunoglobulin A (IgA) vasculitis is a rare entity in adults. It can be triggered by allergens such as drugs, food, or insect bites. We present a case of an adult male with a cutaneous IgA vasculitis of palpable purpura after eating canned sardines.
LEARNING POINTS
- IgA vasculitis with skin involvement is rare in adults.
- It can manifest after exposure to allergens such as drugs and food.
- A good clinical history and thorough anamnesis can lead to a quick diagnosis.
KEYWORDS
Vasculitis, purpura, Henoch-Schönlein, immunoglobulin A (IgA)
CASE DESCRIPTION
A 48-year-old male from Morocco was admitted following referral with abdominal pain and skin lesions on his legs. His past medical history revealed a road traffic accident 20 years earlier that had caused multiple rib fractures, humerus fractures and liver laceration. He had served 11 years in prison for drug dealing. While in prison in 2012, the patient had experienced a ‘rash’ due to the consumption of canned sardines, described as ‘vesicles on the legs’, that disappeared within a few days, leaving hyperpigmented lesions.
In our case, the patient was referred to the emergency department due to abdominal pain and raised and hyperpigmented skin lesions on his legs. Four days earlier, he had eaten canned sardines and the skin lesions reminded him of those that had occurred in 2012. The patient had no fever or other symptoms.
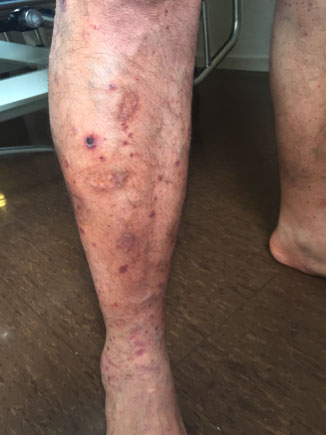
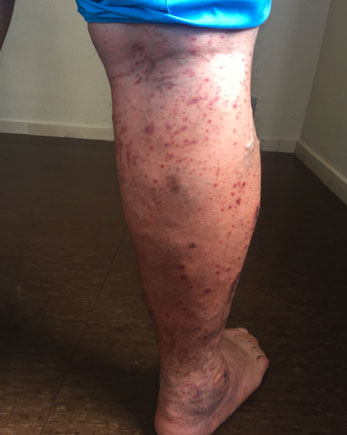
On examination, cardiopulmonary auscultation was rigorously normal. Abdominal palpation presented pain on palpation without focusing on any specific point. Painful and pruritic skin lesions were seen on the buttocks and inferior hemiabdomen in addition to the lower extremities. These were palpable erythematous-violaceous rashes (Figs. 1 and 2).
The patient’s tests were rigorously normal, including renal profile (creatinine, urea, as well as the absence of haematuria or proteinuria), hepatic or hemogram. An autoimmune screen was performed: ANA, ENAs, Anti-DNA, ANCAs and antiphospholipid antibodies, which were all negative. The patient’s proteinogram showed no alteration and serology for CMV, EB, HCV, HBV and HIV was negative.
Given the cutaneous lesions, it was decided to prescribe methylprednisolone 60 mg every 24 hours for 2 days with subsequent oral prednisone 30 mg daily, followed by a reducing regimen. During follow-up the lesions disappeared, leaving hyperpigmented scar lesions.
Figure 1. Anterior view of right leg showing hyperpigmented and raised lesions
Figure 2. Posterior view of right leg showing hyperpigmented and raised lesions
DISCUSSION
IgA vasculitis or Henoch-Schönlein purpura is the most frequent vasculitis in children, affecting 75% of the cases described in children under 10 years of age, with an incidence between 10 and 20 cases per 100,000 population[1,2]. It is much rarer in adults, approximately 10% of all cases, and more prevalent in male patients, depending on the country. In Spain, the prevalence in adults is 25-30%[3].
The aetiology of this vasculitis lacks clarity in literature reviews. There appears to be a type of relationship with certain HLA haplotypes, especially in terms of renal involvement. The triggers are often unknown, having been associated with bacterial and viral infections (e.g. VHZ, VVZ, Parvovirus B19, Yersinia, Shigella, Helicobacter), vaccinations (yellow fever, cholera, typhoid fever) or allergens. These allergens include drugs (penicillin, ampicillin or erythromycin), food, exposure to cold or insect bites. Our case was curious for the fact that the exposure to canned sardines on two occasions had caused the skin lesions to appear. The patient had consumed other canned products previously but without incident.
The most common clinical manifestations of this type of vasculitis are cutaneous lesions in the lower extremity (legs, buttocks, lower abdomen, although it may affect other areas), with symmetric distribution. The typical lesions are erythematous-violaceous, pruritic and exanthematous in nature, appearing as small vesicles or ulcers.
Histologically, perivascular IgA deposits occur; in our case, no biopsy was performed given the improvement of the patient and the benign nature of the process.
Other common manifestations are arthralgia of large joints, gastrointestinal manifestations (abdominal pain, nausea, vomiting, and even rectal bleeding) that occur 8 to 10 days after skin manifestation. However, intussusception in adults is very uncommon. Kidney involvement, present in half of patients affected by this disease, only becomes severe in 10% of cases. It is not coincident with skin involvement and may appear up to 6 weeks later, presenting as isolated haematuria or proteinuria, nephrotic and nephritic syndrome, and even renal failure[4, 5]. Depending on the patient series, end-stage renal disease can be observed in 10-30% of cases at 15 years[6]. There is a series of diagnostic criteria, although the typical cutaneous manifestations are usually diagnostic.
Pharmacological treatment is not necessary and the use of NSAIDs is controversial[7]. The use of corticosteroids at a dose of 1-2 mg/kg should be considered in the case of severe joint and abdominal symptoms. Only in the case of severe renal involvement should immunosuppressants be used.