Keywords
Oxaliplatin, capecitabine, QT prolongation, cardiogenic shock
Abstract
Introduction: Combination-based adjuvant chemotherapy utilising capecitabine and oxaliplatin is widely used in gastric cancer treatment. Rare but severe cardiac events such as prolonged QT, cardiac arrest and cardiogenic shock can result from their use.
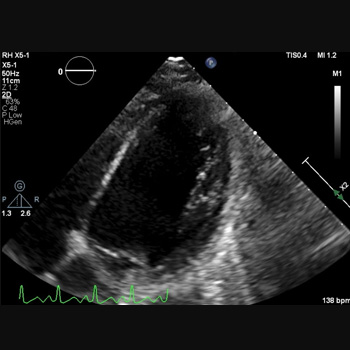
Case description: A 45-year-old female with gastric adenocarcinoma was started on capecitabine-oxaliplatin chemotherapy one week before presenting to the emergency department with weakness. Blood pressure was 78/56 mmHg, heart rate 140 bpm and oxygen saturation 85%. She became unresponsive with pulseless ventricular fibrillation; CPR was initiated with immediate intubation. She received two shocks with a return of spontaneous circulation. Laboratory tests revealed serum potassium (3.1 mmol/l), magnesium (1.1 mg/dl) and troponin (0.46 ng/ml). An EKG revealed sinus tachycardia with a prolonged QT interval (556 ms). The combined effects of capecitabine, oxaliplatin and electrolyte abnormalities likely contributed to the QT prolongation. An echocardiogram demonstrated an ejection fraction of 10%–15%. An emergent right-heart catheterisation showed right atrial pressure of 10 mmHg and pulmonary artery pressure of 30/18 mmHg; cardiac output and index were not recorded. An intra-aortic balloon pump was placed, and she was admitted to the ICU for cardiogenic shock requiring norepinephrine, vasopressin and dobutamine. A repeat echocardiogram showed a significantly improved ejection fraction of 65%, and she was discharged.
Discussion: Capecitabine and oxaliplatin cardiotoxicity is an exceedingly rare occurrence, with both drugs reported to cause QT prolongation.
Conclusion: Healthcare providers must recognise the QT prolongation effects of capecitabine and oxaliplatin, leading to life-threatening cardiac arrhythmias.
References
Views: 435
HTML downloads: 38
PDF downloads: 282
Published:
2024-03-21
Issue:
2024: Vol 11 No 4
(view)










